Wernicke Encephalopathy Learning to Walk Again
Introduction
Wernicke'due south encephalopathy (WE) is an acute neuropsychiatric syndrome resulting from vitamin B1 (thiamine) deficiency (1). The syndrome is characterized past confusion, attentional disorders, incoherence, center-move disorders, and ataxia, although frequently just one or two characteristics are present (2–4). In the industrialized world, most patients with WE accept a background of chronic alcoholism and self-fail (5). Nosotros requires immediate treatment with intravenous or intramuscular thiamine. When patients with We are promptly treated with parenteral thiamine replacement therapy, this is a life-saving measure that also may prevent the development of chronic brain damage (half dozen). When WE is left untreated or is inappropriately treated with either low doses of thiamine or oral thiamine replacement therapy, this may result in a life-threatening situation with bloodshed rates up to twenty% of the patients (four). In the patients who survive with this lack of treatment, varying degrees of brain damage develop, although the exact class of illness is non well-understood (7). Progression into a well-known class of chronic amnesia, Korsakoff'due south syndrome (KS), is non uncommon [Ref. (8), run across Figure one]. Usually, KS follows WE when acute defoliation improves within one to a couple of weeks. Principal characteristics of this improvement include the ability to concentrate for a longer fourth dimension, less incoherence in behavior, and articulate consciousness over the course of the day despite astringent amnesia (8–10).
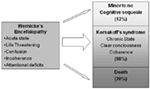
Figure i. Evolution of Wernicke'southward encephalopathy as proposed by Harper et al. (iii) and Day et al. (xi). See Kopelman et al. (8) for a review.
Descriptions of cases of We where the symptoms do not ameliorate rapidly are deficient and often restricted to the acute state of affairs. Examples of such cases accept been described in the course of World War II following starvation in prisoners of war (12). Descriptions of the cognitive sequelae in the course of prolonged defoliation post-obit WE are currently not available in the literature. Such neuropsychiatric descriptions of severe cases of We are crucial, withal, every bit it will give insight in the severity of the syndrome. Despite the current standards of emergency care in the industrialized earth, a vast majority of patients with WE are inadequately managed, resulting in patients who show defoliation for a prolonged time (13–15). Here, nosotros nowadays a example report that illustrates the cognitive and behavioral characteristics, including signs of confusion, of a patient who was admitted to our clinic with untreated We. Neuropsychological cess revealed striking cognitive impairments different KS. Importantly, the initial cognitive and neuropsychiatric problems did not resolve in time, providing an example of a patient with acute WE that became chronic.
Case Written report
Biographical History
According to members of the family unit, the patient functioned independently prior to the neurological problems. The son of the patient visited her several times a week. In her house she was able to manage the household, despite her alcohol abuse. The corporeality of alcohol she consumed varied between one and three bottles of wine each twenty-four hours. She divorced 12 months prior to diagnosis with We. Up until 6 months before admission, the patient worked in a reel kitchen in a hospital. The terminal month, she had non been eating well and consumed alcohol throughout the twenty-four hours. He told that the patient did not feel like eating, but even so spoke about things she wanted to undertake to manage her alcoholism. The 24-hour interval before she was found, she had a telephone call with her son. The son reported that the telephone telephone call included a regular commutation of information without any striking exchange of data.
Medical History
Our patient is a 54-year-former adult female with a 7-twelvemonth history of alcohol abuse. The patient did not have a psychiatric history. She was constitute in her firm on the floor of the living room. Co-ordinate to reports of her son who found her, she was unable to move her legs, showed odd eye movements, had visual hallucinations of food lying effectually her, talked nonsense, and was incontinent of urine. Subsequently a visit of a full general practitioner to her house, her son was told to give his mother residue. After 5 days and no apparent change to her situation, a visiting psychiatrist referred her to the infirmary where she was diagnosed with WE and underwent a therapy of oral thiamine treatment. Afterward, the patient was admitted to a department of an addiction center where she stayed for most 8 months. Here, her beliefs was described as incoherent and confused. She showed a compulsion to visit the toilet regularly and to frequently ask the nursing staff for cigarettes. After her stay in the habit center, she was referred to our dispensary for patients with KS.
Methods
Four months subsequently she was constitute, a neuropsychological evaluation was performed (T1) in the addiction centre. Xvi months after the first evaluation, the cognitive functions were re-evaluated (T2). Results of the showtime and 2nd neuropsychological evaluation are displayed in Table one. A chronic KS reference group is displayed in the last cavalcade. The results for the reference group were adopted from group studies on chronic KS patients as displayed in Tabular array 1. The first neuropsychological evaluation consisted of the Wechsler Adult Intelligence Scale-III (xvi), the Raven Standard Progressive Matrices (17), Word-Fluency Animals and Professions (18), Digit Span Frontward and Backward (xvi), Rey's Complex Figure Task (19), Wechsler Memory Scale-R, Hooper Visual Integration (20), Stroop (21), Trail Making Task (22), and the Behavioral Cess of Dysexecutive Syndrome Key Search Task. The 2nd neuropsychological assessment consisted of the Mini Mental Country Test, the Cognitive Screening Task (23), Word-Fluency Animals, Digit Span Forward and Astern, Trail Making Chore, the Visual Clan Test (24), Rey'south Circuitous Figure Chore and the Frontotemporal Dementia Rating Scale (25). The patient was informed by the first author and asked whether she was willing to participate. Written informed consent was obtained from the legal representative. The procedure was performed in accordance with the guidelines of the Declaration of Helsinki and guidelines for recruitment of incompetent patients [cf. Ref. (26)].
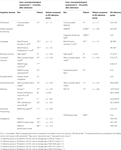
Table 1. Test results of neuropsychological assessment after 4 and 16 months after admission to the infirmary in our case and a KS reference group.
Results
Observations and Neuropsychological Assessment on T1
Qualitative observations on T1 showed a consistent pattern of striking impairments. Mental confusion was reported, with a preference to continue asking for cigarettes, loftier distractibility, and disorganization of beliefs. The patient would often walk abroad during a conversation. Her behavior appeared severely disorganized. While she was sitting behind a computer performing Solitaire, she would move her legs upwardly and downwards vigorously, maybe as a symptom of tardily-phase WE (4). Moreover, she would walk into her room, undress, lay in her bed for simply a couple of minutes. Hereafter she would dress herself, ask the nursing staff for cigarettes, smoke and walk into her room to undress and lay in her bed for just a couple of minutes, and dress over again. During lunch and dinner time, she walked into the room and would merely eat one bite and go out the room instantly. During the nights, she would enquire the staff for nutrient. According to nursing staff reports, she did not show evidence of positive nor negative emotions during the day.
The left column of Table 1 depicts the test scores on neuropsychological assessment afterward 4 months afterwards admission to the infirmary. Initially (T1), her performance on the neuropsychological assessment was consistent with a contour of cognitive deterioration, showing dumb operation on tests for attention, orientation, intelligence, word-fluency, working memory, long-term retentiveness, structure, and executive operation, compared to healthy participants. Chiefly, the cognitive profile was severely affected by the attentional disorders, consistent with an acute WE. Neuropsychological performance ranged from moderate to astringent harm, with the exception of perceptual abilities. The reference groups of KS patients had an impaired operation on orientation, long-term retention, and executive functioning. On tasks intended to index orientation, word-fluency, working memory, visuoconstruction, and intelligence, the performance of the patient was more than one SD below the average score in the KS reference groups. This suggests that both the nature and extent of cognitive disorders in the case study were remarkably serious.
Observations and Neuropsychological Assessment on T2
Qualitative observations of confused behavior lasted during her stay in our Korsakoff clinic without showing any signs of improvement or deterioration over time. The patient appeared as highly distractible if the team members were able to motivate her. She would frequently undress and redress herself in her room.
The correct column of Tabular array 1 depicts the test scores on neuropsychological assessment after sixteen months after access to the hospital. The design of cognitive functioning was consistent to the design of observed cognitive dysfunction at T1. The patient showed similar operation on the cerebral tasks: impaired performance on tests for orientation, intelligence, word-fluency, working memory, long-term memory, construction, attention, and executive functioning compared to salubrious participants. Attentional problems were every bit striking as at T1. The cognitive pattern was stable compared to T1, whereas improvement in case of KS is to be expected based on the available literature (see Figure 1).
Give-and-take
The patient in the present case report showed a distinctive chronic design of cognitive and neuropsychiatric impairments in the course of severe Nosotros. Signs of confusion and breathless behavior were evident and did not resolve in time. Cerebral disorders in attention, long-term memory, working memory, visuoconstruction, and give-and-take-fluency became apparent both after iv and 16 months later access to the hospital. Importantly, the attentional deficits severely afflicted the cognitive profile on both neuropsychological evaluations. Compared to a KS reference grouping, the patient showed a broader range of severe cognitive impairments. The patient was able to role independently upwardly to the point that she adult WE. The cognitive and neuropsychiatric bug were in accordance to the acute symptoms of We and did not improve over the course of her stay in the clinic, suggesting that her WE became chronic.
Wernicke'due south encephalopathy is a life-threatening condition post-obit astute thiamine deficiency (5). Whereas a large bargain of research on Nosotros has been devoted to successful handling of WE in the astute phase, descriptions of cases where confusion does not ameliorate rapidly are currently lacking. This is hit given that in clinical practice, We is undertreated and patients are still admitted to general or psychiatric hospitals with prolonged states of defoliation (13–15). Moreover, Nosotros is potentially fatal in about 20% of the patients (eight). The nowadays example study suggests that WE can non merely result in a life-threatening acute situation, but also in a chronic form of WE, incorporating a chronic country of confusion and disorganized behavior. The severity of the neuropsychiatric symptoms makes a patient in need of lifelong care.
A possible explanation for why the patient in the current case study developed a astringent chronic pattern of cognitive issues could be the belatedly hospital admission and inadequate handling with thiamine replacement therapy. Although the patient was constitute lying on the floor with arable symptoms of neurological disease (e.yard., odd eye movements, visual hallucinations, incontinence), she was not admitted to the infirmary in the showtime v days and received no treatment during this menstruum. Since astringent cognitive disorders are the effect of untreated or under-treated thiamine deficiency, the patient should have received thiamine replacement therapy instantly (7). In the present case, Nosotros was eventually diagnosed in the hospital, later on which oral thiamine supplementation started. This time point of thiamine supplementation is regarded as a very tardily compensation for thiamine deficiency (13). Moreover, oral replacement therapy is less constructive than parenteral replacement therapy (4).
Given that the prognosis of Nosotros is known to depend on the speed of compensating the deficiency in thiamine (xiv) and the severe chronic cognitive disturbance associated with chronic We observed in the present study, our results indicate that an active treatment policy is needed to avert severe chronic neuropsychiatric symptoms. Current treatment standards propose that parenteral (intravenous or intramuscular thiamine should be given 200 up to 500 mg three times daily until symptoms of acute WE resolute (32). In order to foreclose astringent and chronic cognitive disorders, physicians should have a high alphabetize of suspicion for We and dose parenteral thiamine accordingly (seven).
Although the patient in our instance study had a history of alcohol abuse, the neurocognitive symptoms had an acute onset equally reported in We, which makes alcohol dementia an implausible explanation for the severe acute cognitive problems (33). Moreover, the cerebral bug remained stable over a menstruation of 16 months, unlike progressive dementia. Different to KS, the patient had chronic problems in her attentional function, working retentivity, visuoconstruction, and word-fluency functions.
In decision, the electric current case study illustrates the cognitive and behavioral characteristics of a patient who was admitted to our clinic with untreated Nosotros. Our clarification provides the first written report on a patient with prolonged states of defoliation following We, suggesting that WE tin go chronic in case of tardily thiamine replacement therapy.
Conflict of Interest Statement
The authors declare that the research was conducted in the absence of whatsoever commercial or financial relationships that could exist construed as a potential disharmonize of interest.
Acknowledgments
We give thanks the patient and her family unit for their willingness to participate. Tanja C. W. Nijboer was supported by NWO Grant #451-10-013.
References
i. Manzo L, Locatelli C, Candura SM, Costa LG. Nutrition and alcohol neurotoxicity. Neurotoxicology (1994) 15:555–65.
ii. Wernicke C. Lehrbuch der gehirnkrankheiten fur aerzte und studirende. Kassel Theodor Fischer (1881) 2:229–42.
iii. Harper CG, Giles M, Finlay-Jones R. Clinical signs in the Wernicke-Korsakoff complex: a retrospective analysis of 131 cases diagnosed at necropsy. J Neurol Neurosurg Psychiatry (1986) 49:341–v. doi:10.1136/jnnp.49.4.341
Pubmed Abstruse | Pubmed Full Text | CrossRef Full Text
5. Kopelman Physician. Disorders of memory. Brain (2002) 125:2152–xc. doi:10.1093/encephalon/awf229
CrossRef Full Text
eleven. Day East, Bentham P, Callaghan R, Kuruvilla T, George S. Thiamine for Wernicke-Korsakoff Syndrome in people at adventure from alcohol abuse. Cochrane Database Syst Rev (2004) (1):CD004033.
12. De Wardener HE, Lennox B. Cerebral beriberi (Wernicke's encephalopathy): review of 52 cases in a Singapore prisoner-of state of war hospital. Lancet (1947) 1:11–7. doi:10.1016/S0140-6736(47)91272-5
CrossRef Full Text
14. Isenberg-Grzeda E, Chabon B, Nicolson SE. Prescribing thiamine to inpatients with alcohol utilize disorders: how well are we doing? J Addict Med (2014) 8:one–5. doi:10.1097/01.ADM.0000435320.72857.c8
Pubmed Abstract | Pubmed Full Text | CrossRef Full Text
15. Oudman E, Wijnia JW. BNF recommendations for the handling of Wernicke'due south encephalopathy: lost in translation? Alcohol Alcohol (2014) 49:118. doi:10.1093/alcalc/agt179
CrossRef Total Text
16. Uterwijk J. WAIS-Iii Technical Transmission (in Dutch). Lisse: Swets & Zeitlinger (2000).
17. Raven J, Raven JC, Court JH. General Overview. Oxford: Oxford University Press (1995).
18. Mulder JL, Dekker PH, Dekker R. Discussion-Fluency Test (in Dutch). Leiden: PITS BV (2006).
19. Meyers JE, Meyers KR. Rey Circuitous Effigy Test and Recognition Trial (RCFT). Professional Manual. Lutz: Psychological Assessment Resources, Inc. (1995).
xx. Walker RG. The revised hooper visual organisation test as a measure out of brain damage. J Clin Psychol (1956) 12:387–88. doi:x.1002/1097-4679(195610)12:4<387::AID-JCLP2270120421>3.0.CO;two-J
CrossRef Full Text
21. Hammes JGW. De Stroop Color Give-and-take Test Manual (in Dutch). Lisse: Swets en Zeitlinger (1971).
23. de Graaf A, Deelman BG. Cognitive Screening Test Manual (in Dutch). Lisse: Swets & Zeitlinger (1991).
24. Lindeboom J, Schmand B, Tulner L, Walstra K, Jonker C. Visual clan test to detect early dementia of the Alzheimer type. J Neurol Neurosurg Psychiatry (2002) 73:126–33. doi:x.1136/jnnp.73.two.126
Pubmed Abstract | Pubmed Full Text | CrossRef Full Text
26. Meulenbroek O, Vernooij-Dassen M, Kessels RPC, Graff MJL, Sjögren MJC, Schalk BWM, et al. Informed consent in dementia inquiry. Legislation, theoretical concepts and how to assess chapters to consent. Eur Geriatr Med (2010) 1:58–63. doi:10.1016/j.eurger.2010.01.009
CrossRef Full Text
27. Wester AJ, Westhoff J, Kessels RPC, Egger JIM. The Montreal Cerebral Assessment (MoCa) equally a measure out of severity of amnesia in patients with booze-related cerebral impairments and Korsakoff syndrome. Clin Neuropsychiatry (2013) 10:134–41.
28. Oudman Due east, Nijboer TCW, Postma A, Wijnia JW, Kerklaan S, Lindsen Chiliad, et al. Acquisition of an instrumental activeness of daily living in patients with Korsakoff's syndrome: a comparison of trial and mistake and errorless learning. Neuropsychol Rehabil (2013) 23:888–913. doi:x.1080/09602011.2013.835738
Pubmed Abstruse | Pubmed Total Text | CrossRef Full Text
29. Kessels RPC, Kortrijk HE, Wester AJ, Nys GS. Confabulation beliefs and false memories in Korsakoff's syndrome: office of source retentiveness and executive operation. Psychiatry Clin Neurosci (2008) 62:220–v. doi:10.1111/j.1440-1819.2008.01758.x
Pubmed Abstruse | Pubmed Total Text | CrossRef Full Text
thirty. Fujiwara Due east, Brand M, Borsutzky Southward, Steingass H-P, Markowitsch HJ. Cognitive performance of detoxified alcoholic Korsakoff syndrome patients remains stable over two years. J Clin Exp Neuropsychol (2008) xxx:576–87. doi:10.1080/13803390701557271
Pubmed Abstruse | Pubmed Full Text | CrossRef Full Text
32. Thomson Ad, Cook CH, Touquet R, Henry JA. The Royal College of Physicians written report on alcohol: guidelines for managing Wernicke'southward encephalopathy in the accident and emergency department. Booze Alcohol (2002) 37:513–21. doi:x.1093/alcalc/37.vi.513
Pubmed Abstruse | Pubmed Full Text | CrossRef Total Text
33. Oslin D, Atkinson RM, Smith DM, Hendrie H. Alcohol related dementia: proposed clinical criteria. Int J Geriatr Psychiatry (1998) 13:203–12. doi:x.1002/(SICI)1099-1166(199804)xiii:iv<203::Assistance-GPS734>3.0.CO;ii-B
Pubmed Abstract | Pubmed Full Text | CrossRef Full Text
Source: https://www.frontiersin.org/articles/10.3389/fpsyt.2014.00059/full
0 Response to "Wernicke Encephalopathy Learning to Walk Again"
Post a Comment